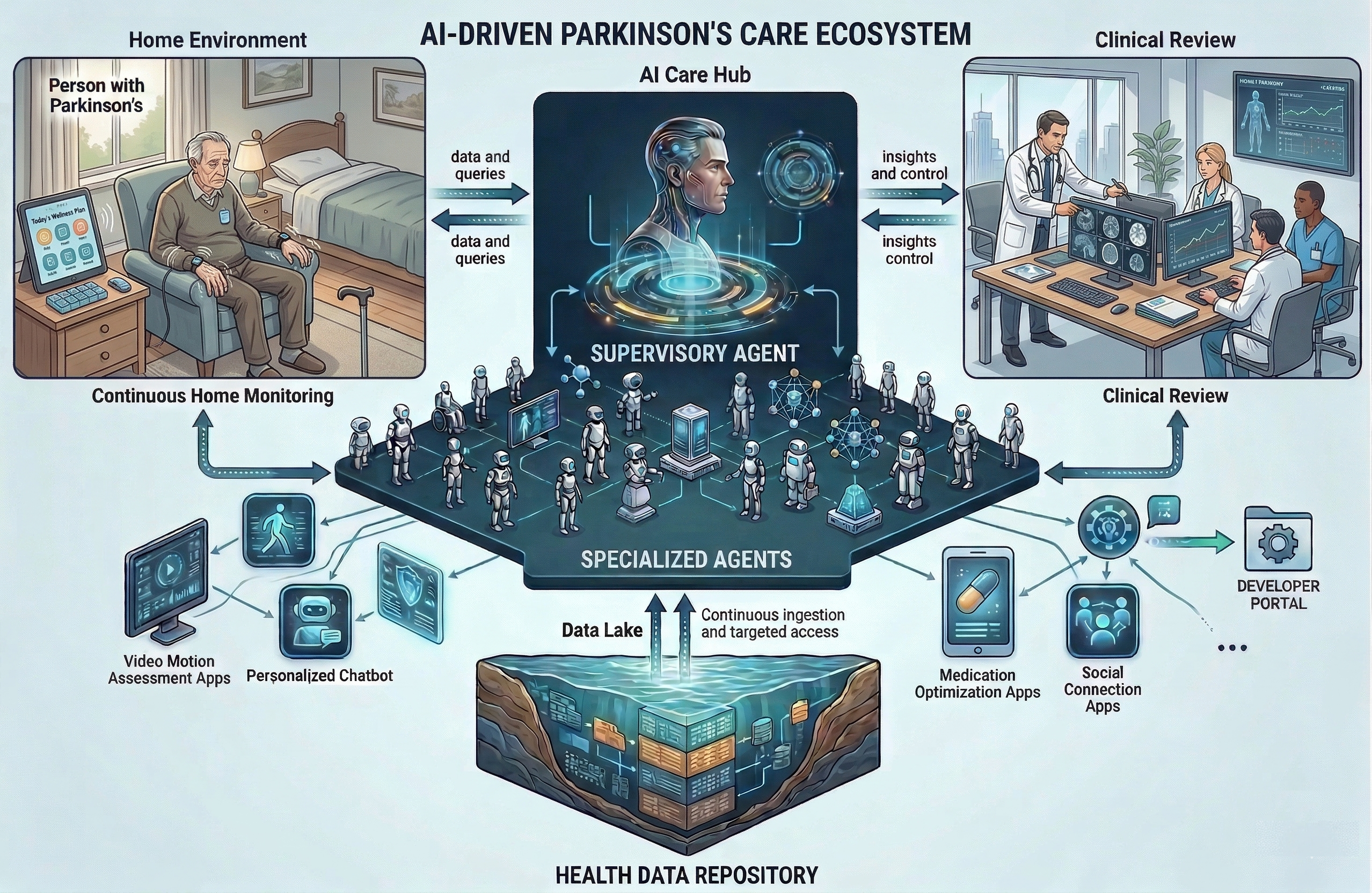
Specialized Agents, Unified Care
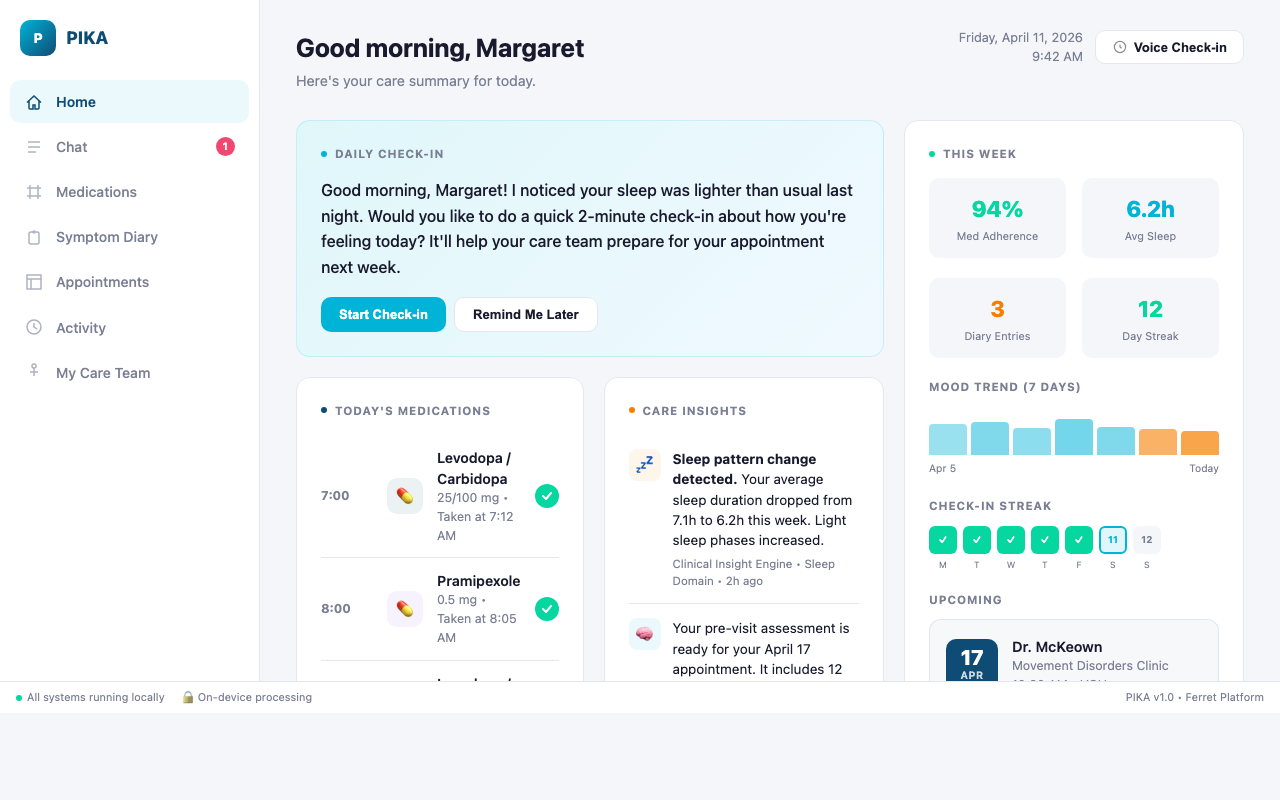
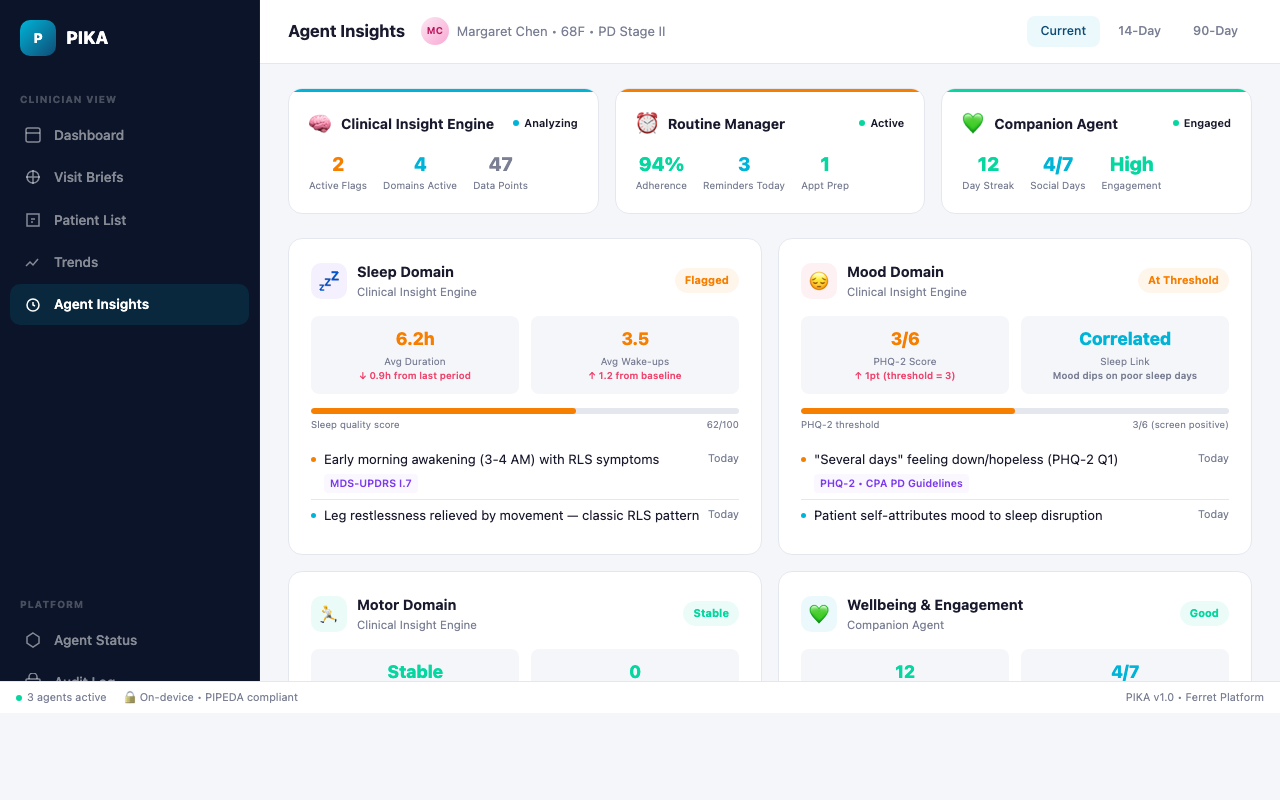
Rather than one monolithic model, PIKA uses purpose-built agents that collaborate through shared memory, each focused on a specific aspect of patient care.
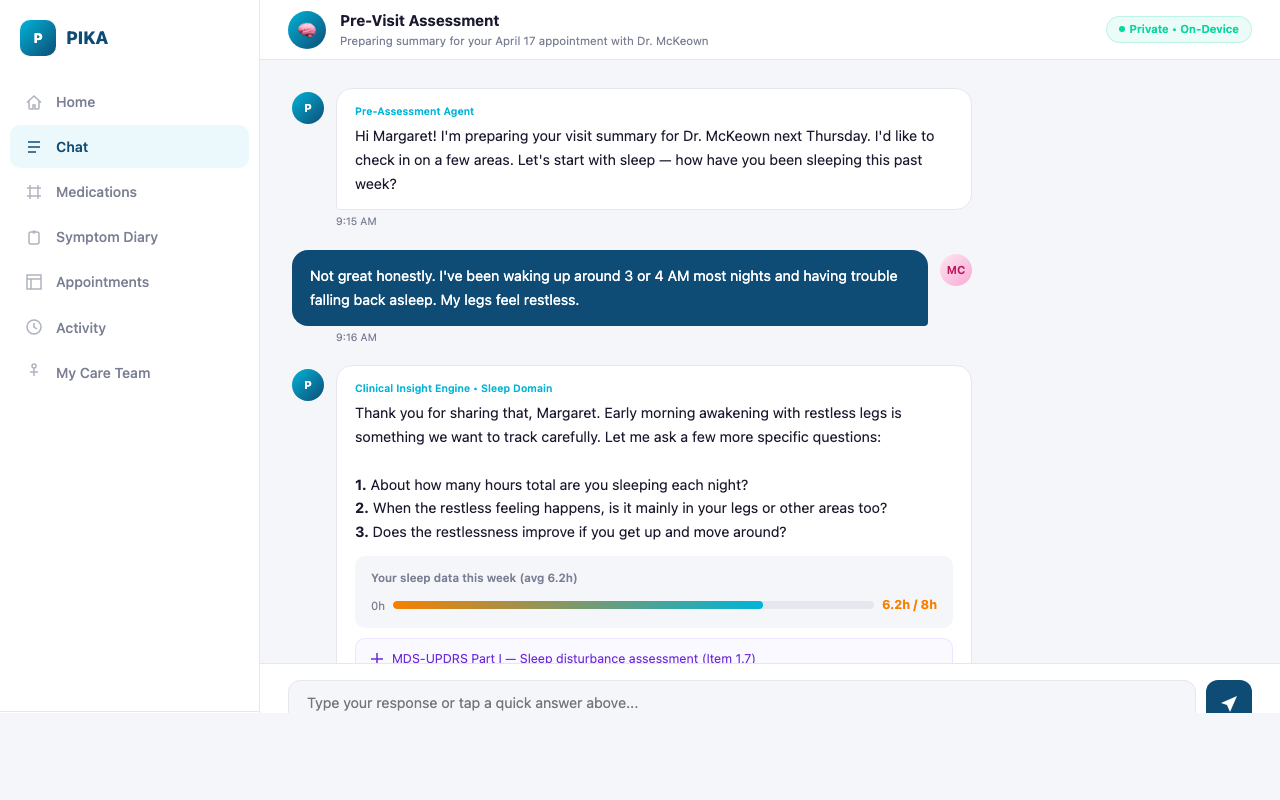
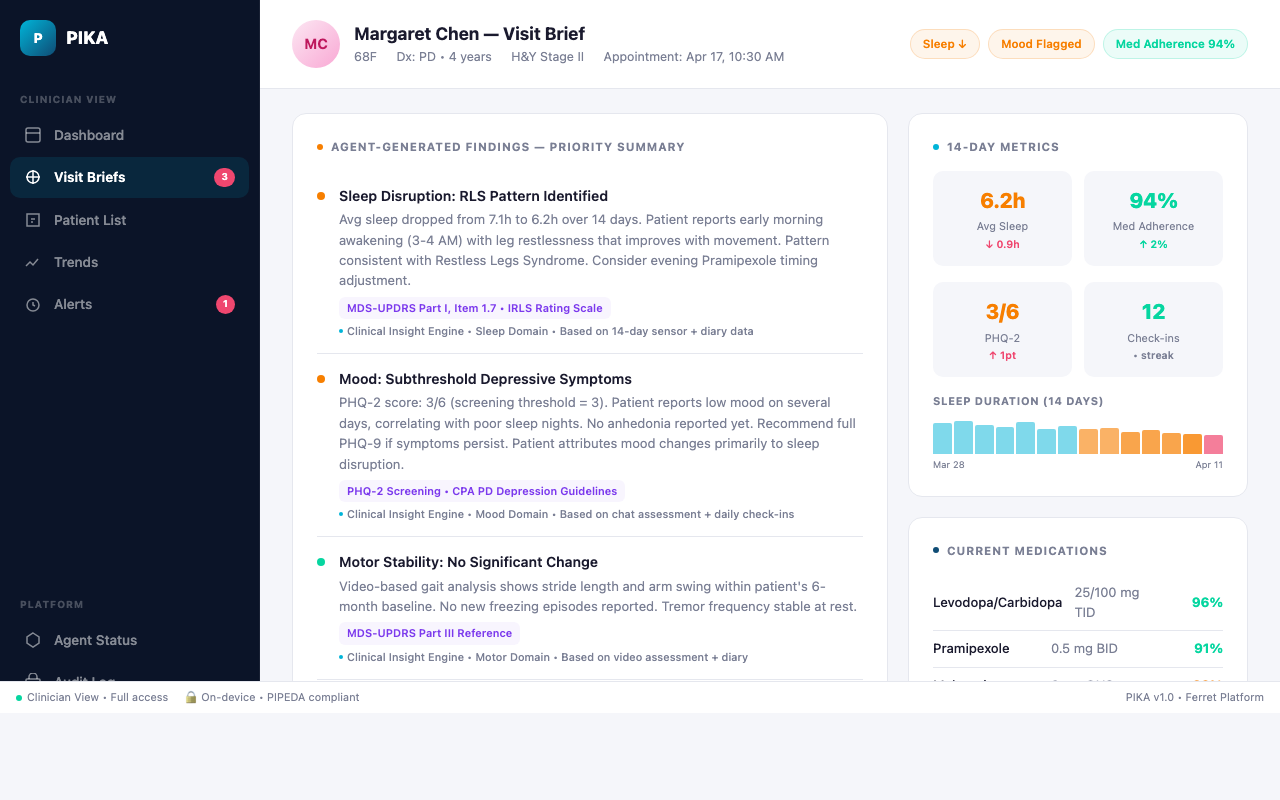
Clinical Insight Engine
Symptom-domain analyzers that evaluate patient data against encoded clinical guidelines
- Mood & Depression (BDI)
- Sleep Disturbance
- Dizziness & Falls
- Hallucinations
Autonomous Routine Manager
Adaptive scheduling and autonomous care workflow management
- Medication Reminders
- Appointment Preparation
- Exercise Prompts
- Portal Navigation
Companion Agent
Daily engagement and psychosocial support to combat isolation
- Daily Check-ins
- Social Connection Nudges
- Positive Reinforcement
- Wellbeing Tracking